Pill Dispensers With Alarms: All You Need to Know

An automatic pill dispenser with alarm is a device that stores your medications, organizes them by dose and time, and alerts you when it's time to take them. If you or someone you love is managing multiple prescriptions and tired of the daily guesswork of "did I already take that?", this kind of device was built for exactly that situation.
Why medication timing matters
Taking medication at the right time is not just a suggestion on the bottle, it directly affects whether the drug works the way it should. Your body absorbs, processes, and eliminates medication on a predictable cycle, and disrupting that cycle has real consequences.10
How your body processes medication on a schedule
When you take a pill, your body moves it through four stages: absorption, distribution, metabolism, and excretion. According to the Orlando Clinical Research Center (OCRC), factors like your age, weight, stomach contents, time of day, and even stress levels affect how quickly your body absorbs a medication and how long it stays active in your system.5 That's why your doctor specifies not just what to take, but exactly when.
Each medication has a therapeutic window. That is the range of time during which the medication is active enough to do its job but not so concentrated that it causes harm. Take a dose too late, and your body may have already cleared the previous dose, leaving a gap with no medication in your system. Take it too early, and the concentration can spike beyond what's safe. The FDA notes that these timing-related interactions become more dangerous when multiple medications are involved, since each drug may alter how the others are absorbed or metabolized.4
The real risk of missed and double doses
Medication errors are more common than most people assume, and they are not limited to home settings. In a landmark study published in the Archives of Internal Medicine, Barker et al. observed medication administration across 36 healthcare facilities and found that 19% of doses contained an error. Of those errors, 43% involved wrong timing and 30% were omitted doses.7 According to AHRQ's Patient Safety Network, adverse drug events account for nearly 700,000 emergency department visits and roughly 100,000 hospitalizations each year in the United States, and about half are preventable.8
These are routine failures in professional care environments with trained staff and standardized protocols. For someone at home managing their own pills without any system at all, the margin for error is even wider.
Who benefits most from an automatic pill dispenser
Automatic pill dispensers with alarms are not just for people who occasionally forget a dose. They are most valuable for people whose daily reality makes consistent medication management genuinely hard. Whether because of the number of pills, physical limitations, or the emotional weight of managing someone else's health from a distance.

Seniors managing multiple medications
The statistics paint a clear picture of why older adults are disproportionately affected by medication management challenges. According to Kaiser Family Foundation (KFF) data, 89% of adults 65 and older are on at least one prescription, and 54% take four or more - a situation doctors call polypharmacy. 1 That kind of regimen (different pills at different times, some with food, some without, some that interact with each other) is a full-time logistical task.
But the challenge goes beyond the number of pills. The CDC reports that nearly half of adults aged 65 and older (47.3%) have been diagnosed with arthritis.2 Arthritis doesn't just cause pain. It makes opening child-resistant pill bottles difficult or impossible. It makes sorting small tablets into tiny compartments painful. It turns a daily routine into a daily physical challenge.
At the same time, according to a study published in the BMJ approximately 40% of people aged 65 and older experience age-associated memory impairment.3 Not dementia, just the kind of normal cognitive decline that makes you uncertain whether you took your morning dose or not. That uncertainty is stressful, and it's dangerous. Double-dosing because you can't remember is a real risk, especially with medications where the margin between effective dose and harmful dose is narrow.10
When you layer these challenges together (multiple medications, painful joints, unreliable memory, and declining vision) the picture becomes clear. This isn't about being forgetful. It's about a set of compounding physical and cognitive changes that make a system functionally inaccessible for the people who need it most.
People with dexterity, vision, or memory challenges
You don't have to be over 65 to struggle with medication management. Anyone living with arthritis, tremors, Parkinson's disease, or chronic pain may find the physical act of opening bottles and sorting pills exhausting or impossible. People with low vision may not be able to read small labels or distinguish between similar-looking tablets.
An automatic dispenser addresses these specific barriers. Rather than requiring you to sort pills by hand each week, the medication management machine handles organization and timing. Many dispensers are designed with accessibility in mind: large buttons, audible and visual alerts, and interfaces that don't require reading fine print. For people with hearing challenges, some models include loud (adjustable) alarms, flashing lights, or the ability to send notifications to a connected phone, so the alert reaches you or your loved one, through whatever channel works best.
Family caregivers managing from a distance
If you are managing a parent's or loved one's medications remotely, you already know the constant low-level anxiety that comes with it. Did they take their morning pills? Did they double up because they forgot? Are they just telling you they took them to avoid the conversation?
For many family caregivers, managing medications is one of the most emotionally difficult parts of the role. An automatic dispenser with app-connected notifications doesn't eliminate that worry entirely, but it changes the dynamic. Instead of calling to check or hoping for the best, you can see whether a dose was taken. If it wasn't, you get a notification — and you can decide how to respond rather than finding out days later at a doctor's visit that the regimen fell apart.
Pill organizers vs automatic dispensers -what's the difference
A standard pill organizer and an automatic pill dispenser solve different problems. Understanding what each one actually does, and what it doesn't, will save you from buying the wrong thing.
Limitations of traditional pill boxes
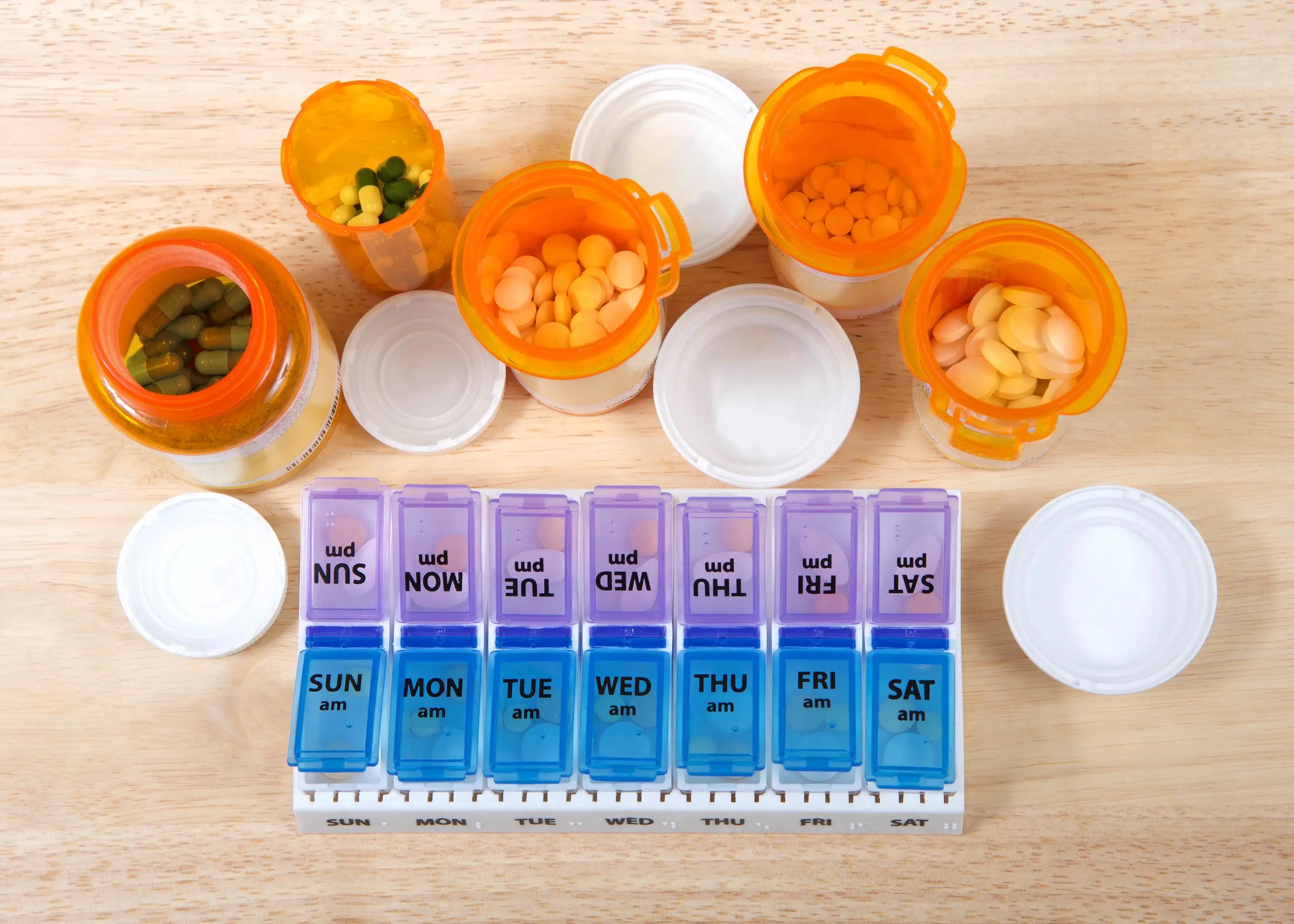
A weekly pill organizer is essentially a storage container with labeled compartments. You (or someone helping you) sorts the medications by hand, typically once a week. It works well enough for people taking one or two pills a day with good dexterity and reliable memory.
For older adults managing complex regimens, the limitations add up quickly. The compartments are often too small for larger pills or multiple medications per time slot. The lids can be difficult to open for someone with arthritis. There are no reminders — if you walk past the box and forget, nothing happens. And if you're refilling weekly, that's 52 opportunities per year for a sorting error that nobody catches until something goes wrong. A pill organizer organizes your pills. It does not manage your medications.
What automatic dispensing actually means
An automatic pill dispenser does what the name implies: it dispenses the correct medication at the correct time, without requiring you to sort, select, or remember. You or a caregiver loads the device (some hold a 30-day supply, others up to 90 days) and the dispenser handles the rest. When it's time for a dose, the device alerts you through sound, light, or a phone notification, and makes only the correct pills available. You don't choose from a grid of compartments. You don't need to read a label or remember which pills go with breakfast. The system knows, and it tells you.
This is a fundamentally different approach from a pill box. It shifts medication management from a manual, error-prone daily task to an automated, monitored system. This is particularly useful when the person taking the medication has any of the physical, cognitive, or logistical challenges described above.
What to look for in a pill dispenser with alarm
Not every automatic pill dispenser is the same. The features that matter most depend on who's using it and what their specific challenges are.
Types of alerts (sound, light, app, caregiver notifications)
The alarm is the entire point of a pill dispenser with alarm, so it needs to actually reach you. Basic models use a simple beep, which is useless if you have hearing difficulties - which is according to a CDC National Center for Health Statistics data brief, affecting approximately 27% of adults aged 65 and older.9
Better models combine multiple alert types: an audible alarm, a flashing light, and a push notification to a phone or caregiver's app. The best systems also escalate; if the first alert is missed, they notify a family member or caregiver automatically rather than just beeping louder into an empty room.
Storage capacity and medication limits
How many medications can the device hold, and how long between refills? A device that holds a week's worth of a single medication is not the same as one that holds a 90-day supply of ten different prescriptions.
For someone managing a complex regimen, fewer refills means fewer opportunities for sorting errors and less burden on the caregiver or family member doing the loading.
Connectivity — offline vs WiFi vs cellular
Low-tech dispensers run on batteries and have no connectivity. They beep at the right time, but nobody knows if the dose was actually taken.
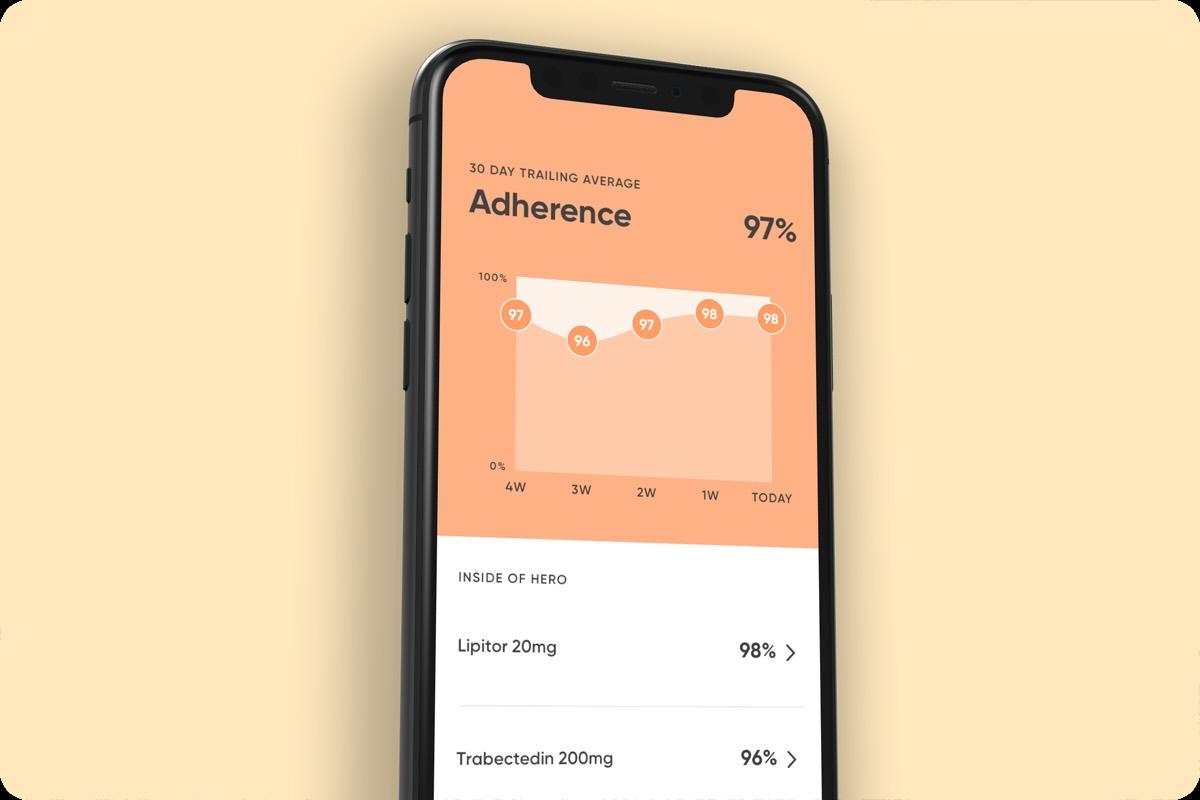
Connected dispensers using WiFi or cellular networks can send real-time data to an app, allowing you or a medication partner to confirm medication adherence remotely. Cellular connectivity has an advantage over WiFi: it works even if the home internet goes down, which matters if the person using the device lives alone.
Security features
If there are other people in the home, especially children or individuals with cognitive impairment, the dispenser should restrict access to medications. Look for locked storage and dispensing that only occurs at scheduled times. An open pill organizer sitting on a counter is an invitation to accidental ingestion. A locked, timed dispenser is not.
Can you trust an automatic pill dispenser?
This is the right question to ask, and the honest answer is: mostly, but with important caveats. No device is perfect, and an automatic dispenser has specific limitations you should understand before relying on one.
Hearing impairments
If the person using the dispenser has significant hearing loss, a sound-only alarm may not work. Make sure the device has visual alerts (flashing lights), vibration, or app-based notifications as backup. A dispenser that relies solely on a beep is a poor choice for anyone over 70, given how common hearing decline is in that age group.
Power outages
Most automatic dispensers plug into a wall outlet. If the power goes out, the device may stop functioning — and if no one is home, a dose could be missed entirely. Some models include battery backup, but not all.
If you live in an area prone to outages, look for a dispenser with an uninterruptible power supply (UPS) option or a safety key that allows manual access to medications during a power failure. This is a simple precaution that is easy to overlook until it matters.
Dementia and severe memory loss
Important: automatic pill dispensers, including Hero, are not recommended for individuals with severe memory loss, Alzheimer's disease, or dementia. A dispenser can alert you that it's time to take your medication, but it cannot ensure that you understand what the alert means or that you follow through correctly. For someone with significant cognitive impairment, a dispenser is not a substitute for hands-on care from a caregiver or medical professional. This is a safety boundary, not a product limitation to work around.
Dispensing accuracy
One reasonable concern is whether the machine itself could make an error, dispensing the wrong pill or the wrong amount. In professional care settings, medication errors are more common than most people assume. A study reviewed by the American Journal of Managed Care (AJMC) found that medication errors in nursing homes affect between 16% and 27% of all residents.6
An automatic dispenser doesn't eliminate the possibility of error (especially during the loading process) but it does remove the daily decision-making that causes most home medication errors. The risk shifts from "did I grab the right pill from the right compartment" to "was the device loaded correctly," which is a less frequent and more controllable event. Hero recommends double-checking your dispensed dose each time, especially if your health depends on it.

How Hero works
If the challenges described in this guide sound familiar, Hero was designed for exactly this situation. Hero is a medication management service, not just a device, that includes three components working together: the award-winning Hero smart dispenser, the Hero app, and 24/7 support.
The Hero smart dispenser holds up to 10 different medications and stores up to a 90-day supply. You load the pills once, set your schedule through the app, and the dispenser does the rest — alerting you at dose time and dispensing your medication.
It supports any pill size or shape, though it is not compatible with half pills, gummies, powdery, sticky, or dissolvable medications. The device is HIPAA compliant and FDA registered.
The Hero app gives you (or a caregiver) real-time visibility into what was taken and when. If a dose is missed, the app sends a notification. For family caregivers managing a parent's medications from across town or across the country, this changes the daily "did Mom take her pills?" uncertainty into actual data. The app also handles schedule adjustments and refill reminders.
Hero's 24/7 support is included with every subscription.
Key takeaways
- Medication timing directly affects whether a drug works safely — missed and mistimed doses are among the most common medication errors, even in professional care settings.
- Older adults face compounding challenges that make manual medication management unreliable: arthritis affects nearly half of adults over 65, 40% experience memory impairment, and more than half take four or more prescriptions daily.
- A traditional pill organizer stores your pills but does nothing to remind you, confirm a dose was taken, or alert a caregiver when something goes wrong — an automatic dispenser does all three.
- When evaluating a dispenser, prioritize connectivity (WiFi or cellular), multiple alert types, and security features — especially if the person using it lives alone or has physical limitations.
- Automatic dispensers are not appropriate for individuals with severe memory loss, Alzheimer's, or dementia — this is a safety boundary, not a feature gap.
Conclusion
Managing medications sounds simple until you're the one doing it. Until you're standing at the counter at 7 a.m. trying to remember if you already took the small white pill or just thought about taking it. Until your hands ache too much to open the bottle. Until your daughter calls for the third time this week to ask if you remembered your evening dose, and you can hear the worry in her voice even though she's trying to sound casual.
An automatic pill dispenser doesn't make the medications go away. It doesn't cure the condition that put you on them. But it takes one complicated, stressful, error-prone part of your day and makes it simpler. It gives you back a small piece of certainty in a situation that often feels uncertain.
That matters more than any feature list.
Complex med schedule?
We solved it.
Hero’s smart dispenser reminds you to take your meds and dispenses the right dose, at the right time.

References
1. Kirzinger, A., Neuman, T., Cubanski, J., & Brodie, M. "Data Note: Prescription Drugs and Older Adults." Kaiser Family Foundation. https://www.kff.org/health-reform/issue-brief/data-note-prescription-drugs-and-older-adults/. 2019.
2. CDC. "Prevalence of Diagnosed Arthritis — United States, 2019–2021." Morbidity and Mortality Weekly Report (MMWR). https://www.cdc.gov/mmwr/volumes/72/wr/mm7241a1.htm. 2023.
3. Small, G.W. "What we need to know about age related memory loss." BMJ. https://pmc.ncbi.nlm.nih.gov/articles/PMC1123445/. 2002.
4. FDA. "Drug Interactions: What You Should Know." U.S. Food and Drug Administration. https://www.fda.gov/drugs/resources-drugs/drug-interactions-what-you-should-know.
5. Orlando Clinical Research Center. "How Does the Body Metabolize Medication?" OCRC. https://ocrc.net/how-does-the-body-metabolize-medication/.
6. Ferrah, N., Lovell, J.J., Ibrahim, J.E. "Nursing Home Medication Errors Are Common but Impact Is Low, Study Finds." American Journal of Managed Care (AJMC). https://www.ajmc.com/view/nursing-home-medication-errors-are-common-but-impact-is-low-study-finds. 2016.
7. Barker, K.N., Flynn, E.A., Pepper, G.A., Bates, D.W., Mikeal, R.L. "Medication Errors Observed in 36 Health Care Facilities." Archives of Internal Medicine. https://pubmed.ncbi.nlm.nih.gov/12196090/. 2002.
8. AHRQ Patient Safety Network. "Medication Errors and Adverse Drug Events." Agency for Healthcare Research and Quality. https://psnet.ahrq.gov/primer/medication-errors-and-adverse-drug-events.
9. Madans, J.H., Weeks, J.D., Elgaddal, N. "Hearing Difficulties Among Adults: United States, 2019." NCHS Data Brief, No. 414. CDC National Center for Health Statistics. https://www.cdc.gov/nchs/products/databriefs/db414.htm. 2021.
Frequently Asked Questions
For many, yes. Unlike a standard box, an automatic dispenser with an alarm helps you access your medication at the scheduled time, which can reduce the risk of error. For a deeper look at your options, see our comparison of pill storage solutions.
For many, yes. Managing multiple prescriptions increases the risk of error. A smart dispenser simplifies complex schedules by organizing and dispensing medication. Learn more about understanding and managing polypharmacy.
Traditional dispensers may just keep beeping, but smart systems can notify a family member or caregiver via an app if a dose is skipped. This is a vital safety net for older adults living independently.
Yes. Hero features a Vacation Mode to dispense meds in advance for a trip, or you can use Travel Mode if you are taking the device with you. For more tips, check out the TSA requirements for traveling with medication.
The contents of the above article are for informational and educational purposes only. The article is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified clinician with any questions you may have regarding a medical condition or its treatment and do not disregard professional medical advice or delay seeking it because of information published by us. Hero is indicated for medication dispensing for general use and not for patients with any specific disease or condition. Any reference to specific conditions are for informational purposes only and are not indications for use of the device.